Bariatric Surgery Abroad: Lithuania
We are one of the leading bariatric surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, Denmark, Germany, Switzerland and other countries.
See before-after pictures
Reviews and Facebook group
Our patients and clinic in the media
Prices
- Gastric bypass – 5.450 £
- Gastric sleeve – 5.450 £
- Gastric band – 3.690 £
- Gastric plication – 3.190 £
- Plastic surgery after a massive weight loss – from 580 £
Regular consultations with Prof. Almantas Maleckas in London
- accommodation with medical care – from 62 £ per night
- plastic surgeon consultation 12 months after surgery (if interested) – FREE
Regular price:
- consultation with the surgeon and anaesthesiologist
- all the necessary health tests before and after the surgery
- bariatric surgery
- anaesthesia
- hospital stay (1-3 days) with 24 hours medical care
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- diet instructions after bariatric surgery
- 10% discount for plastic surgery later (if needed)
- FREE dietician follow-up for 5 years
Please note that the price of the surgery itself is provisional and may be accurately assessed only after the evaluation of each individual case.
The default currency at our clinic is EUR, so if you were looking at prices in GBP it may vary depending on GBP / EUR exchange rate at the moment of payment.
Things to consider when choosing a clinic and surgeon abroad:
- Is it a World-class surgeon with similar experience to ours (700 bariatric surgeries per year) ?
- Is bariatric staff available? We are one of the few clinics that has a specially trained bariatric nursing staff.
- Experience with bariatric anaesthesia? Anaesthesia of overweight patients requires skill and specialised experience, and our anesthesiologists have been specialising in bariatrics for over 15 years.
- What is the quality of the dietitian follow-up services? We offer a 5 year follow-up with a specialised bariatric dietitian.
- Is it a multidisciplinary private hospital? Nordbariatric is a private clinic with modern facilities and exceptional care.
- Overall knowledge in the field? We have designed a unique bariatric mobile app. Our surgeon is the co-author of more than 40 scientific articles.
All of our patients can use one of our offers available at the moment.
- Additional services in our clinic. You or your accompanying persons can explore the various services by following this link. Customise your preferences and request to book any preferred procedures.
- Brand ambassador discount. If you have a community that would be interested in our services, you can now get a discount for your procedure by spreading the word about our clinic on your social media. Contact your customer service representative for more information.
- Recommendation discount. Get a discount for your next plastic or gynaecology procedure by recommending our clinic. Contact your customer service representative for more information.
- Gastric bypass – 6.150 €
- Gastric sleeve – 6.150 €
- Gastric band – 4.200 €
- Gastric plication – 3.600 €
- Plastic surgery after a massive weight loss – from 700 €
Regular consultations with Prof. Almantas Maleckas in London
- accommodation with medical care – from 74 € per night
- plastic surgeon consultation 12 months after surgery (if interested) – FREE
Regular price:
- consultation with the surgeon and anaesthesiologist
- all the necessary health tests before and after the surgery
- bariatric surgery
- anaesthesia
- hospital stay (1-3 days) with 24 hours medical care
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- diet instructions after bariatric surgery
- 10% discount for plastic surgery later (if needed)
- FREE dietician follow-up for 5 years
Please note that the price of the surgery itself is provisional and may be accurately assessed only after the evaluation of each individual case.
The default currency at our clinic is EUR, so if you were looking at prices in GBP it may vary depending on GBP / EUR exchange rate at the moment of payment.
Things to consider when choosing a clinic and surgeon abroad:
- Is it a World-class surgeon with similar experience to ours (700 bariatric surgeries per year) ?
- Is bariatric staff available? We are one of the few clinics that has a specially trained bariatric nursing staff.
- Experience with bariatric anaesthesia? Anaesthesia of overweight patients requires skill and specialised experience, and our anesthesiologists have been specialising in bariatrics for over 15 years.
- What is the quality of the dietitian follow-up services? We offer a 5 year follow-up with a specialised bariatric dietitian.
- Is it a multidisciplinary private hospital? Nordbariatric is a private clinic with modern facilities and exceptional care.
- Overall knowledge in the field? We have designed a unique bariatric mobile app. Our surgeon is the co-author of more than 40 scientific articles.
All of our patients can use one of our offers available at the moment.
- Additional services in our clinic. You or your accompanying persons can explore the various services by following this link. Customise your preferences and request to book any preferred procedures.
- Brand ambassador discount. If you have a community that would be interested in our services, you can now get a discount for your procedure by spreading the word about our clinic on your social media. Contact your customer service representative for more information.
- Recommendation discount. Get a discount for your next plastic or gynaecology procedure by recommending our clinic. Contact your customer service representative for more information.
Patient stories
Only we can offer:
One of the most experienced private bariatric clinic teams in Europe. More than 7.000 bariatric surgeries were performed by our surgeon to this date. A figure that no surgeon or clinic in a region can match.
The only clinic in Europe with a specially designed bariatric mobile app for patients after weight loss surgeries. Available in 6 languages on iOS as well as Android devices.
Watch Peter's gastric bypass story
Bariatric Team

- Our surgeon Almantas Maleckas is a doctor of medical science
- UK General Medical Council (GMC) certified
- He performed over 7.000 bariatric operations
- A pioneer in laparoscopic surgery in the region
- More than 15 years working experience in Sweden, Gothenburg University hospital
- Works both in Lithuania and Sweden, speaks fluent English and Swedish
- London School of Economics graduate

- Our surgeon Nerijus Kaselis is a doctor with a degree in medicine
- Member of the International Federation of Obesity
- Has been practising abdominal surgery for over 32 years, specialising in bariatric surgery for the past 18 years
- Was the first surgeon to perform various laparoscopic surgeries in Lithuania
- Works as a team lead of surgeons in complicated obesity surgeries abroad
- Has international work and study experience

- Our surgeon Linas Venclauskas has over 15 years of experience
- Specialises in minimally invasive surgery, surgical treatment of the upper gastrointestinal tract and bariatric surgery
- Associate Professor at Lithuanian University of Health Sciences
- President of the Kaunas Society of Surgeons
- A member of the European Hernia Society
- Chairman of the Lithuanian Society of Hernia Surgery

- Our surgeon Aurika Karbonskiene has over 25 years of experience as anesthesiologist
- Over 15 years of experience as a bariatric anesthesiologist
- Since 2008 – Associate Professor at Lithuanian University of Health Sciences
- Board member of Lithuanian Society of Anesthesiologists and Intensive Care Physicians
- Member of the European Society of Anesthesiology
- Researcher and coordinator at the Clinical Trial Network of European Society of Anesthesiology

- Our surgeon Almantas Maleckas is a doctor of medical science
- UK General Medical Council (GMC) certified
- He performed over 7.000 bariatric operations
- A pioneer in laparoscopic surgery in the region
- More than 15 years working experience in Sweden, Gothenburg University hospital
- Works both in Lithuania and Sweden, speaks fluent English and Swedish
- London School of Economics graduate

- Our surgeon Nerijus Kaselis is a doctor with a degree in medicine
- Member of the International Federation of Obesity
- Has been practising abdominal surgery for over 32 years, specialising in bariatric surgery for the past 18 years
- Was the first surgeon to perform various laparoscopic surgeries in Lithuania
- Works as a team lead of surgeons in complicated obesity surgeries abroad
- Has international work and study experience

- Our surgeon Linas Venclauskas has over 15 years of experience
- Specialises in minimally invasive surgery, surgical treatment of the upper gastrointestinal tract and bariatric surgery
- Associate Professor at Lithuanian University of Health Sciences
- President of the Kaunas Society of Surgeons
- A member of the European Hernia Society
- Chairman of the Lithuanian Society of Hernia Surgery

- Our surgeon Aurika Karbonskiene has over 25 years of experience as anesthesiologist
- Over 15 years of experience as a bariatric anesthesiologist
- Since 2008 – Associate Professor at Lithuanian University of Health Sciences
- Board member of Lithuanian Society of Anesthesiologists and Intensive Care Physicians
- Member of the European Society of Anesthesiology
- Researcher and coordinator at the Clinical Trial Network of European Society of Anesthesiology
5-year follow up with dietitian
Nutrition is one of the main focus after weight loss surgery to maximize weight loss and prevent weight gain. We offer a dietitian who will talk with you about the diet you’ll need to follow after surgery, explaining what types of food and how much you can eat at each meal. Karolina is a dietitian and Nutrition Consultant with a degree in the medical field. Read more about her here.
Special bariatric app for your mobile phone
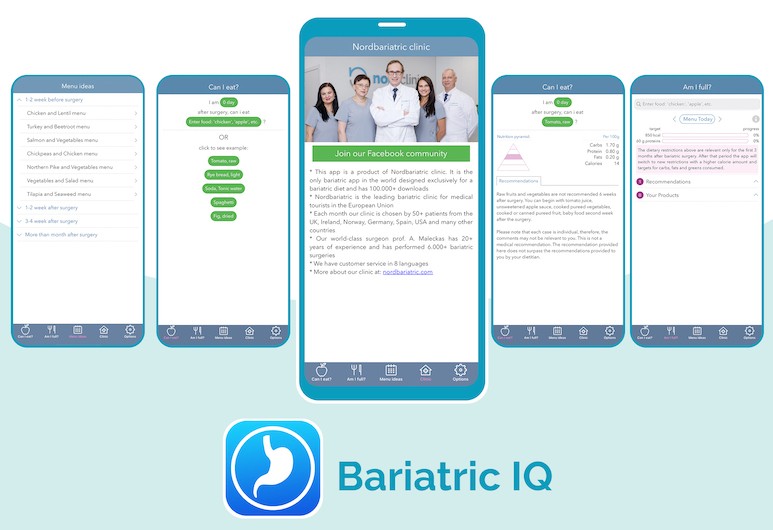
- Created by Nordbariatric clinic
- Special bariatric diet recommendations based on a particular product, a patient’s gender, time after surgery and other factors
- Available in 6 languages
- Available on iOS as well as Android.
- To this date the app was downloaded more than 100.000 times!
- Read more
11 reasons that make us the most popular bariatric clinic abroad
Our team of 3 bariatric surgeons has 15-20 years of experience in the field in total performing over 500 different bariatric surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our leading bariatric surgeon Dr Almantas Maleckas has performed more than 7.000 bariatric surgeries. He is fluent in four languages, among which English and Swedish. The surgeon has been regularly working in Sweden for over 15 years. Dr Maleckas is a pioneer of laparoscopic surgery in Eastern Europe and has trained many other bariatric surgeons in the region.
We are one of the leading bariatric surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, Denmark, Germany, Switzerland and other countries.
We are trusted by our patients and we appreciate all the reviews and feedback collected over the years. Find testimonials here or on Google.
Already more than 5.000 of our former, current and future patients joined our online community with the aim to build a space for opinions and mutual support. Members are welcome to share experiences about their visit to the clinic and to discuss all surgery-related matters.
We offer a 5-year follow-up which includes being able to get in touch with our Lithuanian dietitian Karolina. She is consulting patients after surgery and is available upon request to answer postoperative nutritional questions for five years after surgery.
Our clinic is the only clinic that has developed its own app designed specifically for bariatric patients – Bariatric IQ. The most useful feature of this app is special bariatric diet recommendations based on a particular product, a patient’s gender, time after surgery and other factors. Such a feature has not been replicated by any other bariatric apps in the world. Read more and download the app on your IOS or Android smartphone here.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical services. We care about the safety, comfort and successful results of our patients from all over the world.
The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
We provide customer service in 9 foreign languages including English, Swedish, Norwegian, Danish, Italian, Spanish, French, Russian, Polish. Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
Combining different plastic surgery procedures to offer optimal treatment for post-bariatric patients has been our plastic surgery department’s specialisation for many years now. We have performed such surgeries for more than 10.000 patients to this date. Since weight loss patients often require multiple surgical procedures to address excess skin, surgery planning and surgeons’ experience are very important. We carefully select patients, evaluate each case individually, and only agree to combine surgeries within health & safety limits. Our team of 9 plastic surgeons performs more than 3.000 plastic operations a year, a number that no other clinic in Central & Eastern Europe can match.
Direct flights to Lithuania







What is bariatric surgery?
Bariatric surgery defines a group of surgical interventions which help people lose weight, induce remission of obesity-related diseases, and improve quality of life. A major goal of different bariatric surgeries is the reduction of excess body fat and improvement or remission of co-existing medical conditions, such as type 2 diabetes, cardiovascular diseases, sleep apnoea, osteoarthritis etc. Bariatric procedures are classified as either restrictive or malabsorptive. Restrictive procedures limit intake by creating a small gastric reservoir with a narrow outlet in order to delay emptying. Malabsorptive procedures include excising portions of small intestine where nutrient absorption occurs.
Most popular bariatric surgeries to this date are:
- Gastric bypass (Roux-en-Y gastric bypass, banded gastric bypass, mini gastric bypass)
- Gastric sleeve
- Gastric band
- Gastric plication
FAQ sessions with our surgeon
Watch full list of interview sessions on our Youtube channel.
Why would someone need bariatric surgery?
Obesity is a complex medical condition associated with a great variety of complications which affect most organs through different pathways. There is now considerable evidence that intentional weight loss due to bariatric surgery is linked to clinically relevant benefits for the majority of these health issues.
- First of all, significant weight loss has a positive impact on one’s blood pressure, notably improves cardiac function and reduces risk of cardiovascular events.
- Moreover, it is consistently associated with a clinically relevant reduction in triglycerides and increase in HDL cholesterol, also known as “good” cholesterol.
- Metabolic surgery may be particularly suitable for patients with type 2 diabetes, as these patients may benefit from improved glycaemic control compared to patients treated with medications alone.
- In addition, obesity is widely recognized as a key modifiable risk factor for osteoarthritis, with significant improvements in pain and function reported with weight loss.
- Obstructive sleep apnoea and obesity hypoventilation syndrome tend to improve even when a moderate amount of weight is lost.
- It is worth mentioning that sustained weight loss seems to be associated with a significant improvement in asthma symptoms, too.
- Last but not least, several studies suggest that long-term weight loss not only improves health-related quality of life, but also has a very positive effect on a patient’s self-esteem and so a more positive self-image can be built.
Who is a proper candidate for bariatric surgery?
The most important patient selection criteria for bariatric surgery include body mass index (BMI), the presence of co-morbidities and a history of prior weight loss attempts. Bariatric surgery is advised when BMI ranges from 35 to 40 and there are obesity related conditions such as diabetes or obstructive sleep apnoea, or when BMI is 40 or greater regardless of weight related co-morbidities.
However, an individualized pre-operative assessment is a complex process involving psychological, surgical, dietetic and medical review because benefits of the procedure should outweigh the operative risk for every patient.
It is worth emphasizing that the long-term success of bariatric procedures is critically dependent on patients’ compliance. In order to properly evaluate whether a candidate could make lifelong behaviour changes necessary for sustained weight loss, one must be not only physically, but also psychologically fit to proceed with surgery.
A few pre-existing medical conditions represent absolute contraindications to bariatric surgery. Notable exceptions are unstable coronary artery disease or an advanced liver disease with portal hypertension.
Book a consultation with our surgeon in London
London consultation in:
Don’t miss a chance to book a consultation with our surgeon prof. Almantas Maleckas in London! Read more
What should one expect after bariatric surgery?
A successful weight-loss outcome after bariatric surgery has been defined as a loss of at least 50% of excess weight. Significant weight loss is achieved as caloric intake is reduced by modifying the anatomy of the gastrointestinal tract. However, patients undergoing bariatric surgery often believe they will lose more weight than is consistent with clinical experience and may think that minimal personal effort or risk is involved. Studies have shown that failure to maintain weight loss at 10 years after bariatric surgery has been observed in 10% to 25% of patients who undergo this intervention. The major contributor to poor long-term outcome is non-adherence to dietary and activity recommendations. To assess motivation and predict compliance to postsurgical recommendations, it is advised for patients to lose some weight before surgery. Moreover, psychotropic medications, such as antidepressants, are considered to very likely promote weight gain in post-operative patients.
Lifestyle changes after bariatric surgery
As effective as bariatric procedures are, surgical approach is just a small step forward for more balanced body proportions. Many post-operative adjustments to eating behaviour and daily physical activity routine are needed for successful weight loss and prevention of complications after surgery.
Patients should follow prescribed serving sizes to avoid overeating. Food should be well-chewed and consumed very slowly. Liquids should not be consumed with solid foods.
Moreover, frequent monitoring of nutritional status and additional supplementation, as needed, can aid in preventing severe clinical deficiencies.
Physical activity plays an essential role in weight loss maintenance after a dietary intervention. Several weight loss studies have shown a clear dose response between physical activity and prevention of weight regain.
Possible risks of bariatric surgery
For a more profound understanding about bariatric surgery its risks should be assessed along with the significant benefits. Postoperative gastrointestinal complications of bariatric surgery are common.
Nausea and vomiting occur in more than 50% of patients undergoing restrictive procedures, partly as a result of eating too much or too rapidly but sometimes because of anastomotic stricture or other mechanical consequences of the operation.
The dumping syndrome, a complex of neurohormonally mediated symptoms that include facial flushing, lightheadedness, palpitations, fatigue, and diarrhoea, occurs in some patients after Roux-en-Y gastric bypass. Typically triggered by the ingestion of concentrated sugar, this syndrome may discourage patients from eating foods with a high sugar content, thus contributing to the beneficial effects of the operation.
Deficiencies of iron, calcium, folate, vitamin B12, and other nutrients occur after procedures with a component of malabsorption, such as gastric bypass. With the more extensive procedures, such as biliopancreatic diversion, protein malnutrition and deficiencies of the fat-soluble vitamins (A, D, E, and K) may occur. All of these deficiencies require regular monitoring and replacement.
Other gastrointestinal complications include dehydration, bowel obstruction, anastomotic leaks, strictures, erosions, ulcers, adhesions, internal and incisional hernias, and cholelithiasis.
Cardiopulmonary complications, such as myocardial infarction and pulmonary embolism, although rare, are the major causes of mortality, representing about 70 % of all perioperative deaths.
In addition, studies have shown that the most serious surgical complication of the commonly performed bariatric surgeries, such as gastric bypass, is anastomotic leakage which may potentially lead to life-threatening peritonitis.
All things considered, patients at a higher risk for perioperative and postoperative complications are males, smokers, and those with higher BMI, older age or multiple comorbidities.
How to prepare for bariatric surgery?
Right preparation for bariatric surgery is a vital part of the procedure itself as it determines the success of the operation and the quality of recovery after it.
- Practice healthy lifestyle. Exercising regularly, having your diet balanced and staying hydrated will strengthen your body and recovery after the surgery will be faster.
- Avoid using tobacco products and consuming alcohol at least 1 month before the procedure.
- In order to prevent perioperative complications, taking aspirin, anti-inflammatory drugs and other blood thinners should be avoided at least 2 weeks before the procedure, unless the operating doctor has advised otherwise.
- Consult the surgeon about your allergies, previous surgeries and daily medications. If you have any pre-existing conditions that require daily usage of drugs, your operating doctor should be informed about it.
- Follow your specific pre-operative instructions as they may vary depending on your personal medical history.
When weight loss surgery doesn't work. Possible reasons
Although bariatric surgery is often recommended as an effective treatment for severe obesity, there is still variability in outcome. There are 3 most commonly observed factors that might adversely affect the results of a bariatric procedure: binge eating, lowered energy metabolism, and psychosocial functioning.
Binge eating behaviour, which is characterized by episodes of eating an objectively large amount of food and feelings of loss of control, may occur after the surgery and is tightly associated with weight regain through overeating. There are several patterns of eating disturbance that also often occur among post-surgery patients who have regained weight: continuous snacking, eating large quantities of sweet foods, and consuming large quantities of soft or liquid foods. In this case, patient’s determination to stay in shape plays a major role in altering one’s pre-existing eating habits.
However, eating behaviour is controlled at least partially by mechanisms governing energy metabolism, which, in turn, govern energy expenditure, too. In order not to regain weight after the surgery, it is extremely important that excess calories from food are turned into actual mechanical energy. Therefore, staying at least minimally active is extraordinarily important for those who undergo bariatric surgery.
Last but not least, nowadays psychological disturbances are considered to be of paramount importance in the development of obesity and, conversely, the efforts to treat obesity that are not accompanied by resolution of psychological factors may lead to a deterioration of mental health and failure of treatment.
Taking everything into account, improvement in general health status, long-term changes in eating behaviour, and psychosocial adjustment are the most important factors that define a positive outcome of a bariatric procedure. For it to be truly successful patient’s determination and wilful seek for changes are of utmost importance.
Most popular bariatric surgery methods these days, a quick overview of the methods
Roux-en-Y gastric bypass is often referred to as a combined restrictive–malabsorptive procedure. It involves stapling of the stomach to create a small (≤30.0 ml) upper gastric pouch. The small intestine is then divided and the distal portion (called the alimentary, or Roux, limb) is attached to the gastric pouch. The distal portion of the stomach and proximal small intestine (the biliopancreatic limb) are connected farther down the jejunum. Food comes into contact with pancreatic and biliary enzymes only below this connection site. In this way less food is eaten and not all of it can be absorbed.
Adjustable gastric banding is a restrictive procedure that involves placing a silicone implant around the top of the stomach. The inner part of this band contains a balloon that can be filled with saline at any time through a virtually painless injection though the skin, providing partial obstruction to the flow of food and allowing less food to be comfortably eaten. Food slowly passes through the band into the remainder of the stomach.
Sleeve gastrectomy is a restrictive procedure in which the stomach is transected vertically creating a gastric tube and leaving a pouch of 100 to 200 ml. The main aim of this procedure is similar to that of an adjustable band which is portion control. It is worth noting that in this case no intestinal rearrangement as in gastric bypass surgery and no foreign body placement as in adjustable gastric banding is required.

- Created by Nordbariatric clinic
- Special bariatric diet recommendations based on a particular product, a patient’s gender, time after surgery and other factors
- Available in 6 languages
- Available on iOS as well as Android.
- To this date the app was downloaded more than 100.000 times!
- Read more
11 reasons that make us the most popular bariatric clinic abroad
Our team of 3 bariatric surgeons has 15-20 years of experience in the field in total performing over 500 different bariatric surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our leading bariatric surgeon Dr Almantas Maleckas has performed more than 7.000 bariatric surgeries. He is fluent in four languages, among which English and Swedish. The surgeon has been regularly working in Sweden for over 15 years. Dr Maleckas is a pioneer of laparoscopic surgery in Eastern Europe and has trained many other bariatric surgeons in the region.
We are one of the leading bariatric surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, Denmark, Germany, Switzerland and other countries.
We are trusted by our patients and we appreciate all the reviews and feedback collected over the years. Find testimonials here or on Google.
Already more than 5.000 of our former, current and future patients joined our online community with the aim to build a space for opinions and mutual support. Members are welcome to share experiences about their visit to the clinic and to discuss all surgery-related matters.
We offer a 5-year follow-up which includes being able to get in touch with our Lithuanian dietitian Karolina. She is consulting patients after surgery and is available upon request to answer postoperative nutritional questions for five years after surgery.
Our clinic is the only clinic that has developed its own app designed specifically for bariatric patients – Bariatric IQ. The most useful feature of this app is special bariatric diet recommendations based on a particular product, a patient’s gender, time after surgery and other factors. Such a feature has not been replicated by any other bariatric apps in the world. Read more and download the app on your IOS or Android smartphone here.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical services. We care about the safety, comfort and successful results of our patients from all over the world.
The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
We provide customer service in 9 foreign languages including English, Swedish, Norwegian, Danish, Italian, Spanish, French, Russian, Polish. Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
Combining different plastic surgery procedures to offer optimal treatment for post-bariatric patients has been our plastic surgery department’s specialisation for many years now. We have performed such surgeries for more than 10.000 patients to this date. Since weight loss patients often require multiple surgical procedures to address excess skin, surgery planning and surgeons’ experience are very important. We carefully select patients, evaluate each case individually, and only agree to combine surgeries within health & safety limits. Our team of 9 plastic surgeons performs more than 3.000 plastic operations a year, a number that no other clinic in Central & Eastern Europe can match.
Our clinic

Self-catered accommodation with medical care
Send us your enquiry








